On November 3rd, we were honored to accept the 2017 Delaware Valley Patient Safety & Quality Award from The Health Care Improvement Foundation for our submission, “Implementation of a Patient Blood Management Program,” which outlines the integration of patient blood management (PBM) as a daily, embedded quality improvement strategy at Thomas Jefferson University Hospitals (TJUH). The project was evaluated on evidence of significant and sustained improvement in quality, patient safety, innovation, and the potential for replication in other healthcare organizations. As an outsourced provider of PBM implementation, we are thrilled to share in TJUH’s success and we applaud its leadership and organizational commitment to improvement.
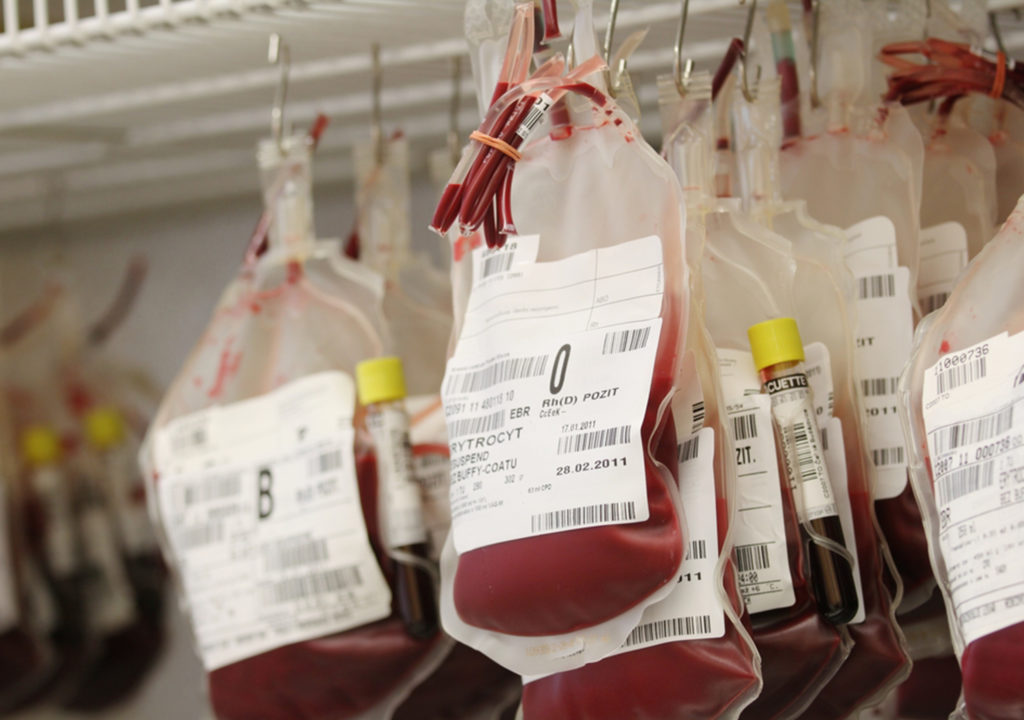
In healthcare, the sweet spot is the perfect balance of healthcare spending and patient outcomes. It’s the place of equilibrium that features just the right type and degree of patient care while avoiding the cost and potential harm of unnecessary interventions. Some providers have learned that balancing both clinical and economic concerns must begin on the most basic level—with a check of the patient’s blood health—and implementation of effective patient blood management (PBM) strategies.
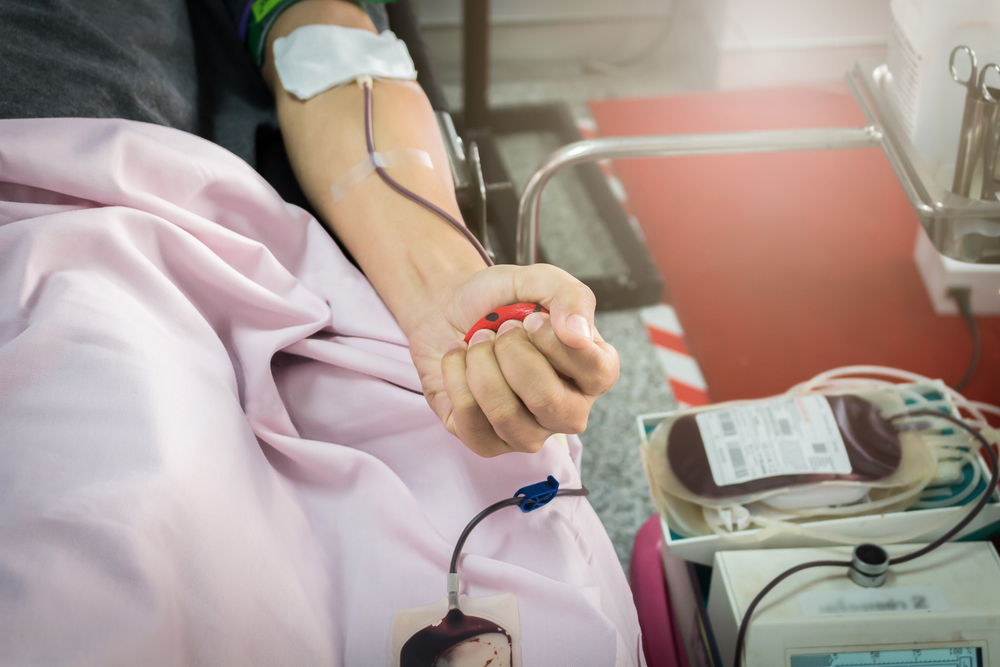
Both the American Medical Association and The Joint Commission consider red blood cell transfusion to be among the five most overused procedures, yet it remains one of the most commonly performed medical interventions in U.S. hospitals today. Vague clinical guidelines and long-held norms have created wide variation in the use of transfusion, but many administrators and clinicians are now realizing that reducing transfusion rates with evidence-based patient blood management programs can provide significant clinical and economic benefits.

Recently I attended the 2017 Annual Meeting of The American Academy of Cardiovascular Perfusion. The AACP, as always, offered strong educational content and a great opportunity to meet up with friends and colleagues. While there, I had the pleasure of presenting co-authored research on “The Effectiveness of Acute Normovolemic Hemodilution and Autologous Prime on Intraoperative Blood Management during Cardiac Surgery.” The AACP honored our team, which includes our perfusion associates and their tireless dedication to clinical excellence and data collection, by selecting this work as the meeting’s Best Paper. I encourage you to read the abstract for additional detail, but here’s a summary of our findings, which highlight the value of thoughtful perfusion strategies that can reduce the need for costly transfusions and increase the likelihood of better clinical outcomes.




