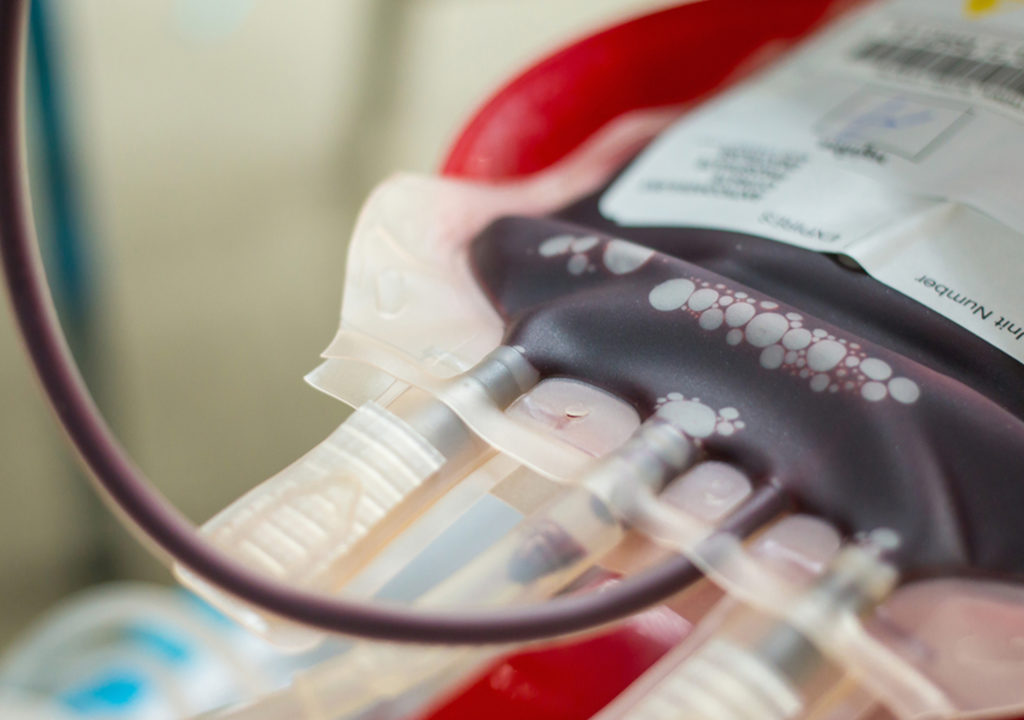
On November 3rd, we were honored to accept the 2017 Delaware Valley Patient Safety & Quality Award from The Health Care Improvement Foundation for our submission, “Implementation of a Patient Blood Management Program,” which outlines the integration of patient blood management (PBM) as a daily, embedded quality improvement strategy at Thomas Jefferson University Hospitals (TJUH). The project was evaluated on evidence of significant and sustained improvement in quality, patient safety, innovation, and the potential for replication in other healthcare organizations. As an outsourced provider of PBM implementation, we are thrilled to share in TJUH’s success and we applaud its leadership and organizational commitment to improvement.
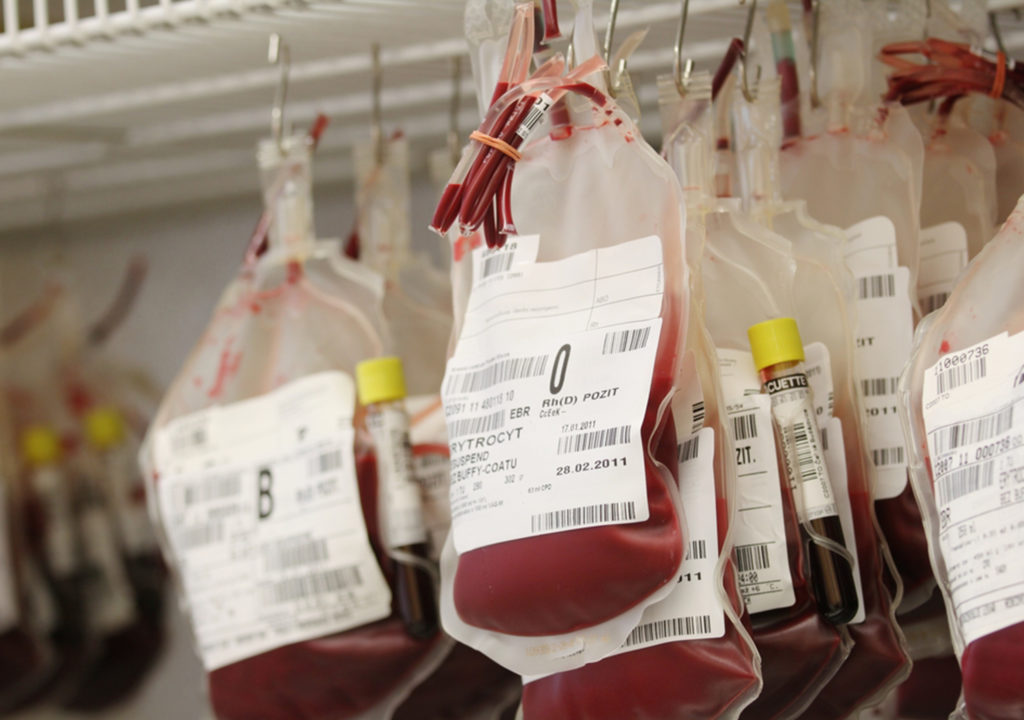
In healthcare, the sweet spot is the perfect balance of healthcare spending and patient outcomes. It’s the place of equilibrium that features just the right type and degree of patient care while avoiding the cost and potential harm of unnecessary interventions. Some providers have learned that balancing both clinical and economic concerns must begin on the most basic level—with a check of the patient’s blood health—and implementation of effective patient blood management (PBM) strategies.
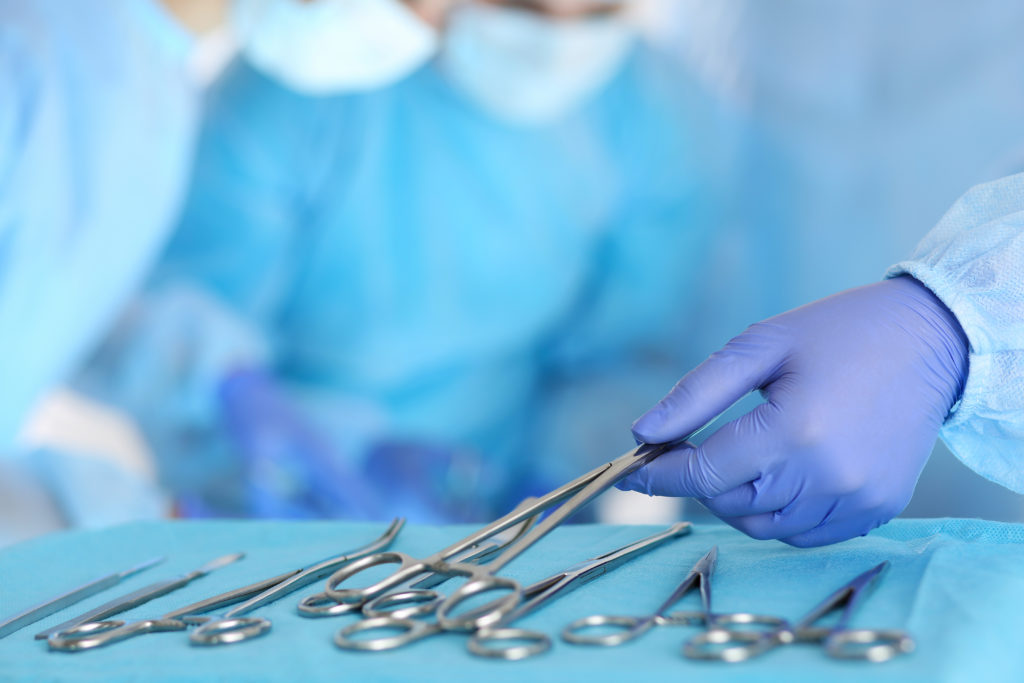
Imagine you’re riding a bicycle that slips a chain. It’s a basic fix, but you have to stop pedaling to do it. When your sterile processing chain slips, you don’t get to stop, and it’s very difficult to fix the bike yourself while you’re still pedaling. Hospital administrators and managers focused on continuous improvement are increasing attention on their sterile processing departments to improve quality, efficiency, surgeon satisfaction, and patient care. An outside sterile processing consultant who has the expertise to conduct a useful assessment and create and implement strategic plans can quickly jump start a quality improvement program without disrupting the department’s regular activities. This is a significant advantage over an in-house approach to improvement. As a result, many leading hospitals are engaging expert consultants for help.

It is a fairly well-known fact in the cardiac community that women have higher morbidity and mortality associated with coronary artery bypass (CABG) procedures. The reasons traditionally given for this disparity include women’s relatively smaller vasculature, higher incidence of anemia, and smaller circulating blood volume. Early in 2016, we in the Medical Department were discussing this phenomenon and decided to design a study using the robust data from our SpecialtyCare Operative Procedural Registry to find something in the intraoperative space that might be leading to these very different post-operative outcomes for men and women. Our findings were somewhat surprising.
Excellence in sterile processing management is fundamental to a well-run operating room. It supports on-time starts, surgeon satisfaction, and overall efficiency—all of which translate to financial results. But, most importantly, effective sterile processing management reduces the occurrence of healthcare-acquired infections (HAIs), which can significantly harm the patients entrusted to your care.