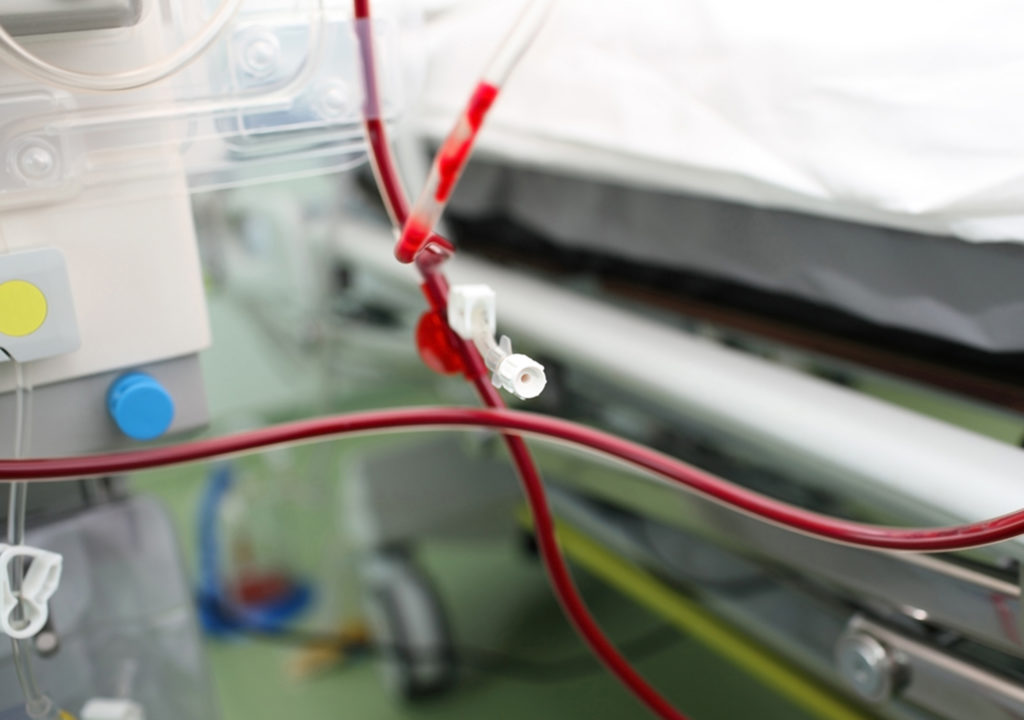
The risks and complications of blood transfusion are well documented. One technique commonly used to help reduce the need for bank blood is autotransfusion, also referred to as intraoperative autotransfusion (IAT) or autologous blood transfusion. IAT is a method of collecting the patient’s blood lost during surgery, processing it, and returning it to the patient. This can significantly reduce, or even eliminate the need for blood transfusions, which in turn reduces complications and the cost of care.
On November 3rd, we were honored to accept the 2017 Delaware Valley Patient Safety & Quality Award from The Health Care Improvement Foundation for our submission, “Implementation of a Patient Blood Management Program,” which outlines the integration of patient blood management (PBM) as a daily, embedded quality improvement strategy at Thomas Jefferson University Hospitals (TJUH). The project was evaluated on evidence of significant and sustained improvement in quality, patient safety, innovation, and the potential for replication in other healthcare organizations. As an outsourced provider of PBM implementation, we are thrilled to share in TJUH’s success and we applaud its leadership and organizational commitment to improvement.
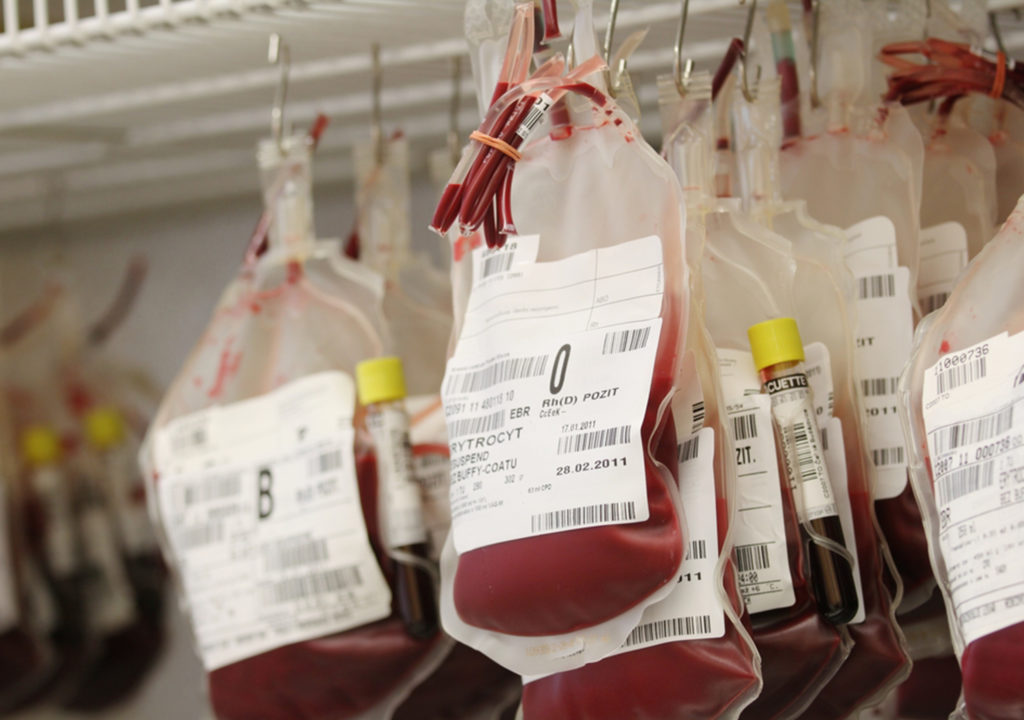
In healthcare, the sweet spot is the perfect balance of healthcare spending and patient outcomes. It’s the place of equilibrium that features just the right type and degree of patient care while avoiding the cost and potential harm of unnecessary interventions. Some providers have learned that balancing both clinical and economic concerns must begin on the most basic level—with a check of the patient’s blood health—and implementation of effective patient blood management (PBM) strategies.

Parts of the United States are experiencing record-breaking heat this summer, and yet, icebergs are everywhere! Icebergs—the classic metaphor for situations wherein most of the substance (and risk) hide below the surface—have been used to discuss topics as varied as psychology, homelessness, big data, influence, safety, Hemingway, and school performance. Risks hidden below the surface are prevalent in healthcare, too. When teams assess their clinical outcomes, some factors are clear and measurable. These parts of the iceberg are above the surface, and hospitals increasingly are held accountable for them. Other outcomes, or factors that affect outcomes, are lurking within the complexity of hospital operations but are demonstrably significant in the future health of the patient.
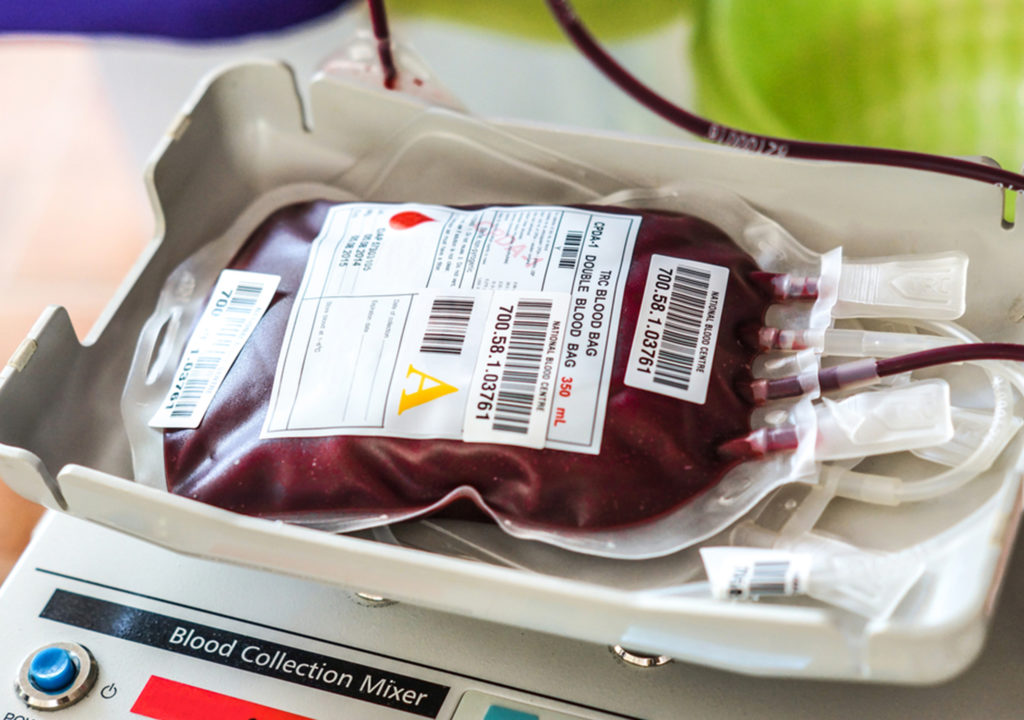
Evidence-based patient blood management (PBM) strategies offer significant clinical benefits. Conservation techniques, in particular, help minimize the use of allogeneic red blood cell transfusion, which has been shown to increase the risk of postoperative complications, readmissions, and mortality among patients. Because of the importance of this area of study, SpecialtyCare researchers continue to drill down and analyze the perfusion and autotransfusion cases in SCOPE, the SpecialtyCare Operative Procedural Registry™, to examine the impact of various strategies, develop best practices, and improve patient outcomes.
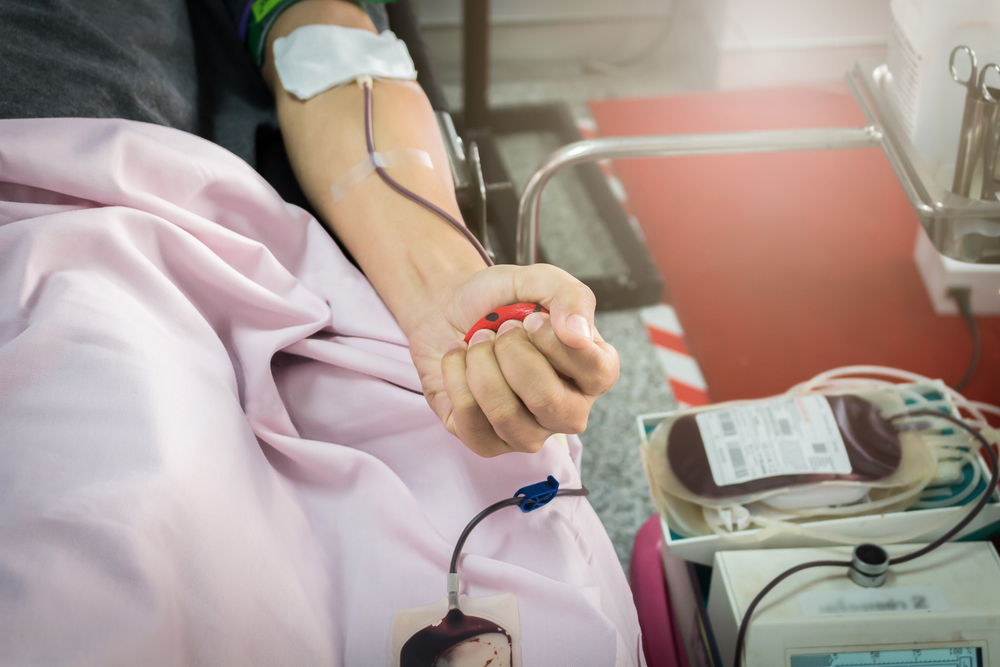
Both the American Medical Association and The Joint Commission consider red blood cell transfusion to be among the five most overused procedures, yet it remains one of the most commonly performed medical interventions in U.S. hospitals today. Vague clinical guidelines and long-held norms have created wide variation in the use of transfusion, but many administrators and clinicians are now realizing that reducing transfusion rates with evidence-based patient blood management programs can provide significant clinical and economic benefits.

AORN 2017 was the place to be for perioperative registered nurses and others who share a continuing commitment to quality care. Nurses, and the hospitals they represent, are constantly looking for ways to improve patient outcomes while also reducing the cost of care. Both of these goals were addressed in some of the most talked-about educational sessions and posters presented during the conference. Cost containment and better clinical outcomes were also recurring themes among the 600 attendees who visited our booth. In addition to exhibiting, we hosted an educational networking dinner that featured a presentation on one of healthcare’s hottest topics—patient blood management (PBM).



