
Parts of the United States are experiencing record-breaking heat this summer, and yet, icebergs are everywhere! Icebergs—the classic metaphor for situations wherein most of the substance (and risk) hide below the surface—have been used to discuss topics as varied as psychology, homelessness, big data, influence, safety, Hemingway, and school performance. Risks hidden below the surface are prevalent in healthcare, too. When teams assess their clinical outcomes, some factors are clear and measurable. These parts of the iceberg are above the surface, and hospitals increasingly are held accountable for them. Other outcomes, or factors that affect outcomes, are lurking within the complexity of hospital operations but are demonstrably significant in the future health of the patient.
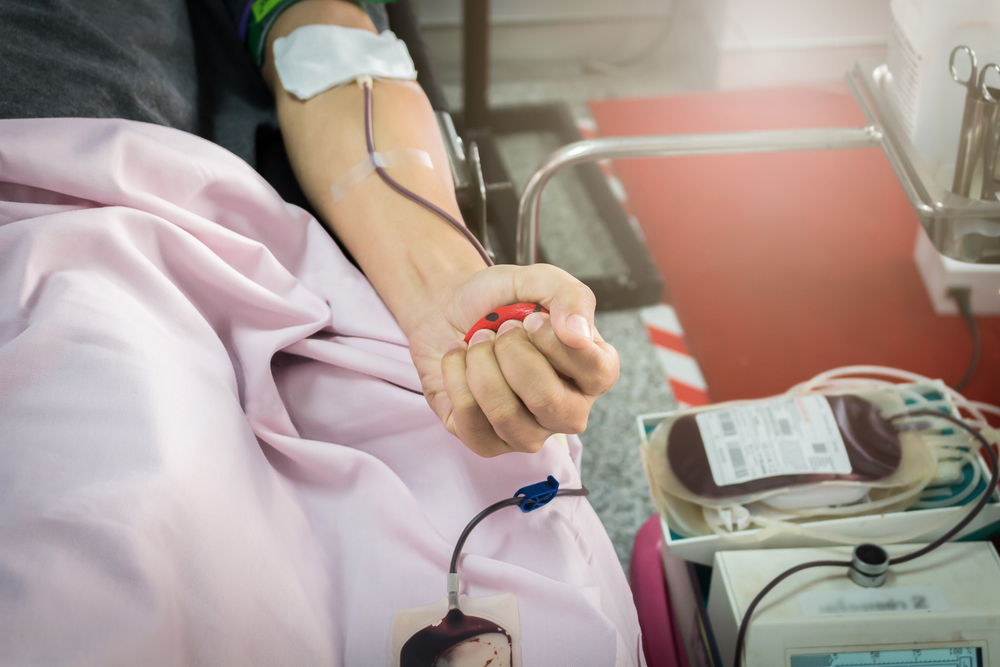
Both the American Medical Association and The Joint Commission consider red blood cell transfusion to be among the five most overused procedures, yet it remains one of the most commonly performed medical interventions in U.S. hospitals today. Vague clinical guidelines and long-held norms have created wide variation in the use of transfusion, but many administrators and clinicians are now realizing that reducing transfusion rates with evidence-based patient blood management programs can provide significant clinical and economic benefits.

Perfusion is an integral part of your hospital’s cardiovascular care program, but the overhead costs and administrative burden of maintaining and managing a team of reliable perfusionists with advanced skills can pose challenges for program administrators. It can be easy, however, to overlook both the indirect costs and benefits of clinical services. So, whether your perfusion is handled in-house or outsourced, we’ve developed a new guide, The Real Spend of Your Perfusion Program: Twelve Tips to Discover the True Value, to help you evaluate your program and any changes that you might be considering.

Changes in reimbursement models are driving changes in operations, including data collection and reporting. Providers are being encouraged and incentivized to implement value-based care (VBC) that emphasizes cost savings and quality outcomes instead of the traditional fee-for-service (FFS) reimbursement model that pays according to the number of procedures performed. The idea is that when hospitals have financial incentives to be accountable for patient outcomes, then the comprehensive focus on quality will result in overall lower costs. Transitioning from FFS to VBC may be especially difficult for ORs with their high costs of procedures, but several strategies can help clear the path to progress.

From a healthcare perspective, the only thing we can be certain of in 2017 is that there will be uncertainty. For healthcare administrators, there is uncertainty around how to manage changes in provisions of the Affordable Care Act, Bundled Payments for Care Improvement (BPCI), and the Medicare Access and CHIP Reauthorization Act (MACRA). Restructuring Medicare and Medicaid could have a significant impact on planning, implementation, and payments for providers. But, regardless of the new format, healthcare providers like SpecialtyCare will always have an obligation—both to their patients and their customers—to improve value by providing high-quality care while containing costs.

On October 26, 2016, SpecialtyCare acquired Sentient, a highly regarded intraoperative neuromonitoring provider. We’re thrilled to welcome the people of Sentient to our team. We believe we’ll be a great fit together, both clinically and culturally. Combining our talent and experience will enhance our collective strengths and create new opportunities to advance patient care and drive clinical quality, which reduce costs for our patients and customers.

Sylvia Burwell, Secretary of the Department of Health and Human Services (HHS), is tasked with transforming our healthcare system from a fee-for-service model to a value-based system driven by the goals of access, affordability, and quality. Initiatives and legislation linked to Medicare, Medicaid, and other programs, such as the Health Insurance Marketplace and the Patient Protection and Affordable Care Act, have all but upended our healthcare system, sending providers, payers, and patients scrambling to understand and manage the changes.

Estimates vary when calculating the money lost to fraud—it’s difficult to measure that which is undetected—but the Federal Bureau of Investigation (FBI) states that healthcare fraud costs the country tens of billions of dollars each year. Paying for law enforcement, legal resources, and sophisticated technology to combat the problem adds to the price tag. Taxpayers and employers endure the financial brunt of fraud, but illegal schemes can also put patient health at risk. Clearly, healthcare fraud is not a victimless crime.

