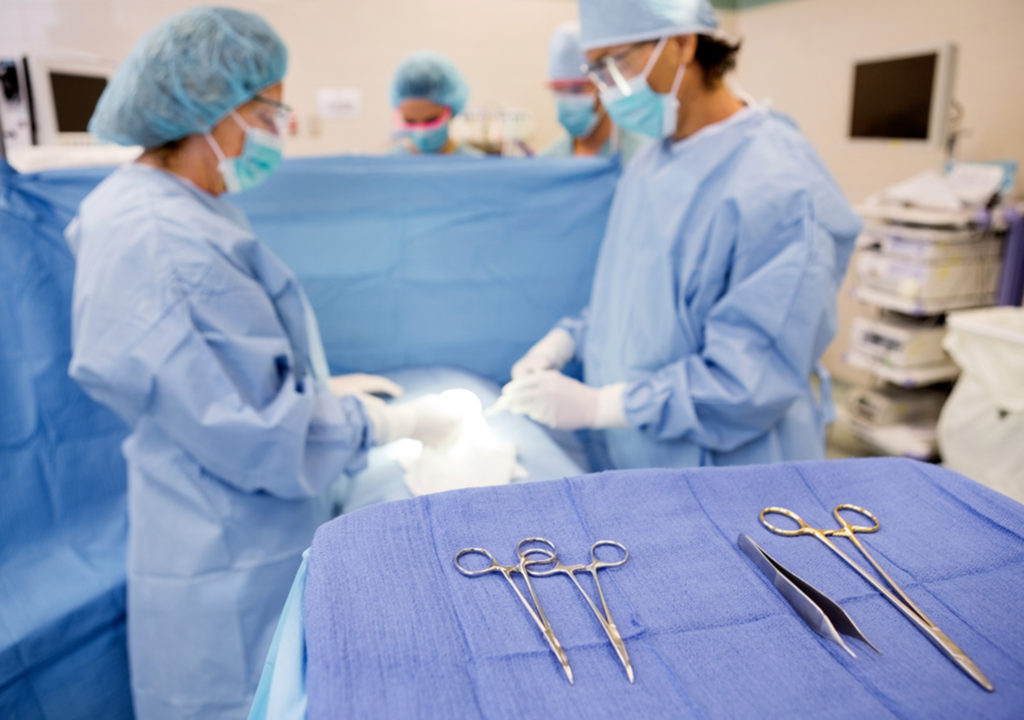
Data-driven, metric-based healthcare is required in today’s value-based environment and essential for sound decision-making. Without it, you’re simply guessing. Cost reductions and real increases in volume, efficiency, and ultimately revenue can be achieved when data and analytics are at your fingertips. That’s why we are excited to introduce SpecialtyCare OptimizeOR™, a user-friendly decision support and analytics system that helps OR managers improve productivity in perioperative performance. OptimizeOR software pulls your key performance measures into an easy-to-use online interface so that you can better manage resources for improved scheduling, staff allocation, and supply utilization. Optimized resource management makes space for increased case volume, minimizes inefficiency, reduces unnecessary spending, and drives patient and surgeon satisfaction.

Parts of the United States are experiencing record-breaking heat this summer, and yet, icebergs are everywhere! Icebergs—the classic metaphor for situations wherein most of the substance (and risk) hide below the surface—have been used to discuss topics as varied as psychology, homelessness, big data, influence, safety, Hemingway, and school performance. Risks hidden below the surface are prevalent in healthcare, too. When teams assess their clinical outcomes, some factors are clear and measurable. These parts of the iceberg are above the surface, and hospitals increasingly are held accountable for them. Other outcomes, or factors that affect outcomes, are lurking within the complexity of hospital operations but are demonstrably significant in the future health of the patient.
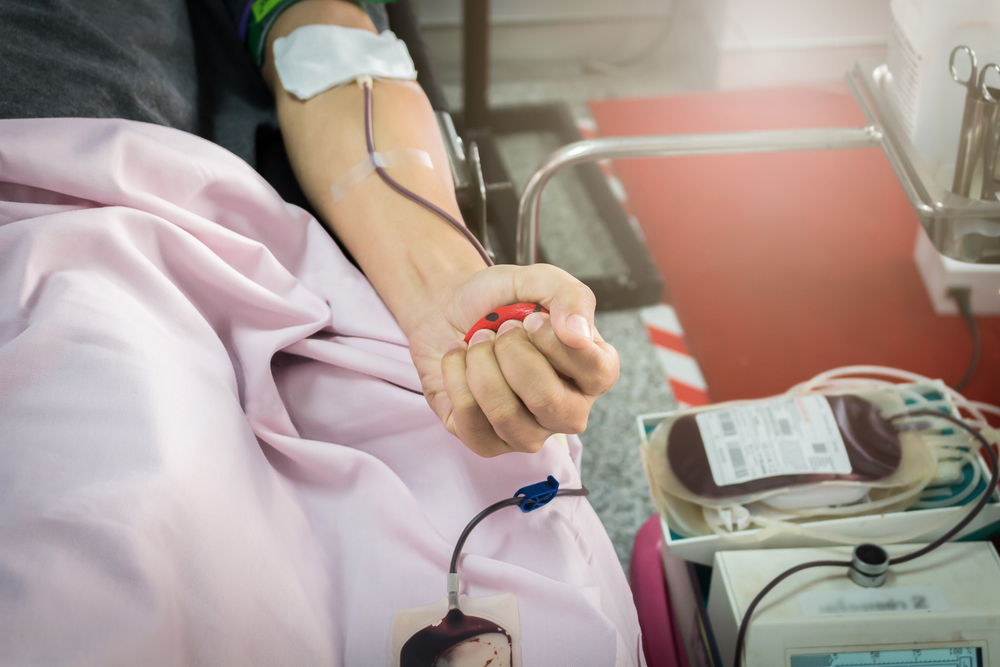
Both the American Medical Association and The Joint Commission consider red blood cell transfusion to be among the five most overused procedures, yet it remains one of the most commonly performed medical interventions in U.S. hospitals today. Vague clinical guidelines and long-held norms have created wide variation in the use of transfusion, but many administrators and clinicians are now realizing that reducing transfusion rates with evidence-based patient blood management programs can provide significant clinical and economic benefits.

AORN 2017 was the place to be for perioperative registered nurses and others who share a continuing commitment to quality care. Nurses, and the hospitals they represent, are constantly looking for ways to improve patient outcomes while also reducing the cost of care. Both of these goals were addressed in some of the most talked-about educational sessions and posters presented during the conference. Cost containment and better clinical outcomes were also recurring themes among the 600 attendees who visited our booth. In addition to exhibiting, we hosted an educational networking dinner that featured a presentation on one of healthcare’s hottest topics—patient blood management (PBM).

A complex system offers a lot of places to hide bad behavior. Medicare and Medicaid—programs at the heart of the current healthcare debate—are particularly vulnerable to violations of Stark Law, the Anti-Kickback Statute, and the False Claims Act. Nearly every day, the Office of Inspector General (OIG) issues details of individuals and hospitals being charged or convicted of healthcare fraud and abuse. Financial penalties and the possibility of imprisonment aside, damning headlines can destroy the bottom line and reputation of even the most respected providers. Compliance violations drive up healthcare costs and compromise patients who are overcharged or subjected to unnecessary tests and treatments.

Consolidation in healthcare is nothing new, in fact it’s hotter than ever. Most analysts, and others who know the industry well, will tell you this trend is positive as we seek better patient outcomes, operational efficiencies, and cost containment to deliver higher value care. In the outsourced medical service provider sector of healthcare, we also can increase value with mergers and acquisitions. As the sector matures, consolidation offers new opportunities to provide customers with high quality, specialized, and reliable services that support hospitals’ goals within today’s rapidly changing healthcare environment.

Recently I attended the 2017 Annual Meeting of The American Academy of Cardiovascular Perfusion. The AACP, as always, offered strong educational content and a great opportunity to meet up with friends and colleagues. While there, I had the pleasure of presenting co-authored research on “The Effectiveness of Acute Normovolemic Hemodilution and Autologous Prime on Intraoperative Blood Management during Cardiac Surgery.” The AACP honored our team, which includes our perfusion associates and their tireless dedication to clinical excellence and data collection, by selecting this work as the meeting’s Best Paper. I encourage you to read the abstract for additional detail, but here’s a summary of our findings, which highlight the value of thoughtful perfusion strategies that can reduce the need for costly transfusions and increase the likelihood of better clinical outcomes.

Changes in reimbursement models are driving changes in operations, including data collection and reporting. Providers are being encouraged and incentivized to implement value-based care (VBC) that emphasizes cost savings and quality outcomes instead of the traditional fee-for-service (FFS) reimbursement model that pays according to the number of procedures performed. The idea is that when hospitals have financial incentives to be accountable for patient outcomes, then the comprehensive focus on quality will result in overall lower costs. Transitioning from FFS to VBC may be especially difficult for ORs with their high costs of procedures, but several strategies can help clear the path to progress.

It’s been said that “Everyone has a special talent, some are just flashier than others.” And so it is in healthcare. Behind every high-visibility physician and hands-on surgical team, there is a large group of people in back offices providing invaluable support. Everyone plays an important role—from human resources and training to accounting and scheduling. But today, as part of National Medical Staff Services Awareness Week, we proudly recognize our credentialing team at SpecialtyCare, and indeed in healthcare settings everywhere, for their contributions to quality patient care and safety.

